BetterBirth Report Addendum: Special Topics on Complication Management
Worldwide, it is estimated that about 85% of babies spontaneously initiate breathing at the time of birth, while 10% respond to drying and stimulation, 3% respond to supportive ventilation with a bag and mask, and 2% require additional support such as intubation.
These numbers are higher for groups such as premature newborns.16 Any facility offering childbirth services must be able to provide resuscitation; it is an emergent complication that cannot wait for a referral.
Findings
Learnings about process
In BetterBirth facilities, 6.4% of newborns whose birth was observed (184/2,869) were resuscitated with a neonatal bag and mask. We analyzed the characteristics of the women and newborns who received resuscitation at the study facilities
(excluding referrals) to understand if there were any notable differences.
We found that only a slightly higher percentage of low birthweight and preterm newborns received resuscitation compared with normal weight, term newborns. The rate is surprisingly low, as particularly preterm newborns are more likely to require respiratory support. Other trends showed that a higher percentage of first children received resuscitation (11.4%) versus 3.2% of babies from women with 4+ parity, which may reflect a social bias against these women.
Figure 10. Percentage of infants who received resuscitation with bag and mask, by core characteristics
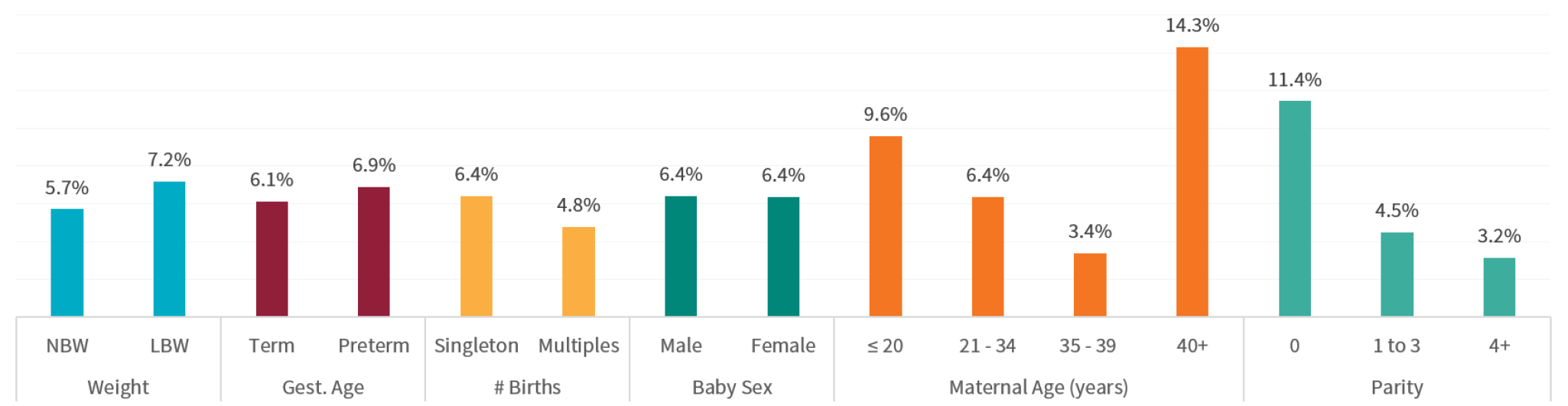
Learning about health outcomes
Within seven days of birth, 20% of the newborns followed in our primary outcomes who received resuscitation died—primarily from asphyxia and complications of prematurity (e.g., lung underdevelopment). Within the subset of newborns studied in our verbal autopsy work, among those who died within seven days of birth and did not receive resuscitation (n=62), the primary causes of death were asphyxia (39%), complications of prematurity (21%), and sepsis (19%).
Figure 11. Risk of perinatal mortality among patients who received resuscitation with a bag and mask versus not, by core characteristics
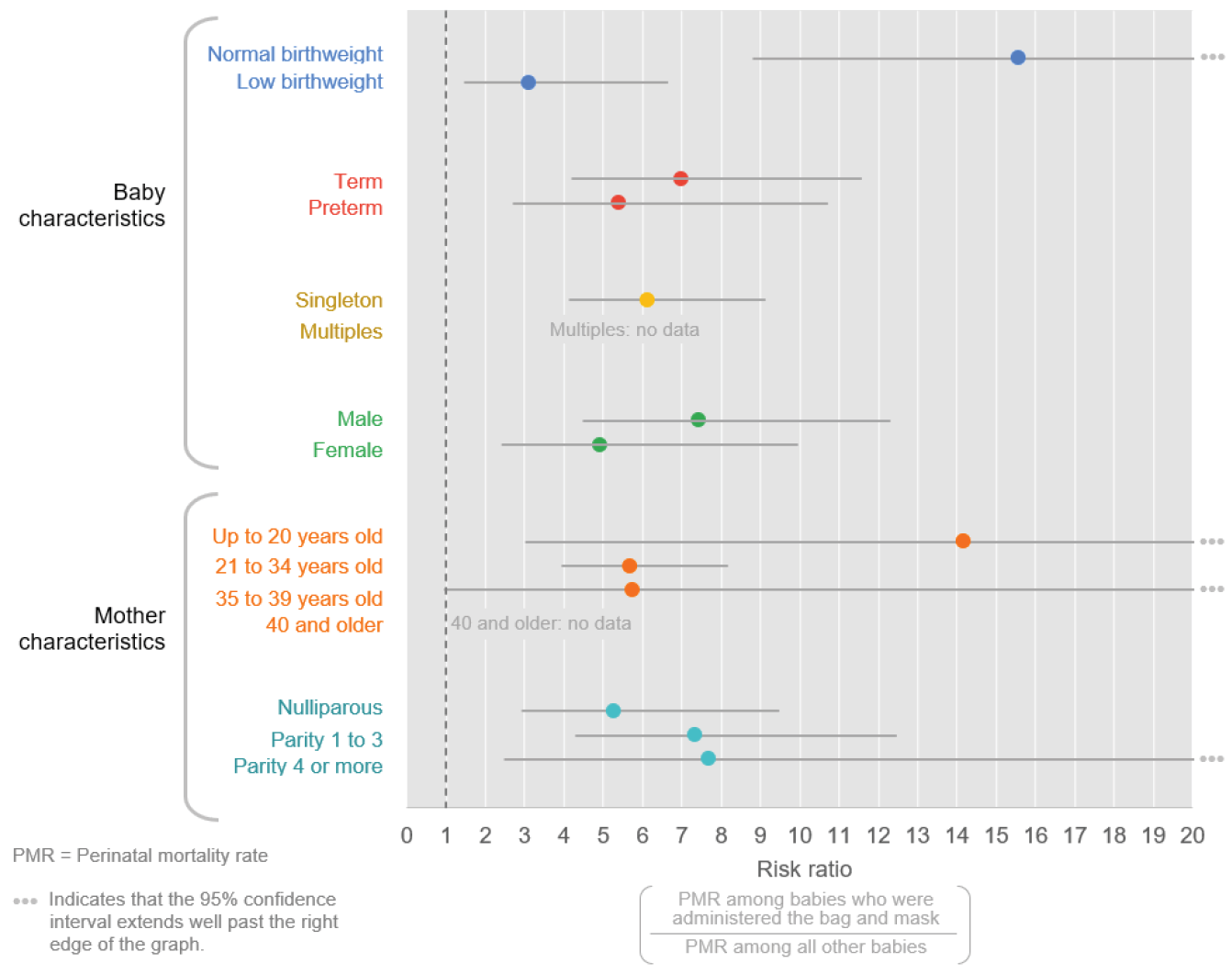
In looking closer at the risk ratio across various groups (Figure 11), we can see that the risk of perinatal mortality among normal birth weight babies who received resuscitation care was more than 15 times higher, while the risk was 3 times higher for low birthweight newborns who were resuscitated. This may indicate that resuscitation efforts by birth attendants are less effective among normal birth weight newborns, or potentially that the PMR for low birthweight newborns is so high overall that resuscitation does not greatly impact mortality. ■


